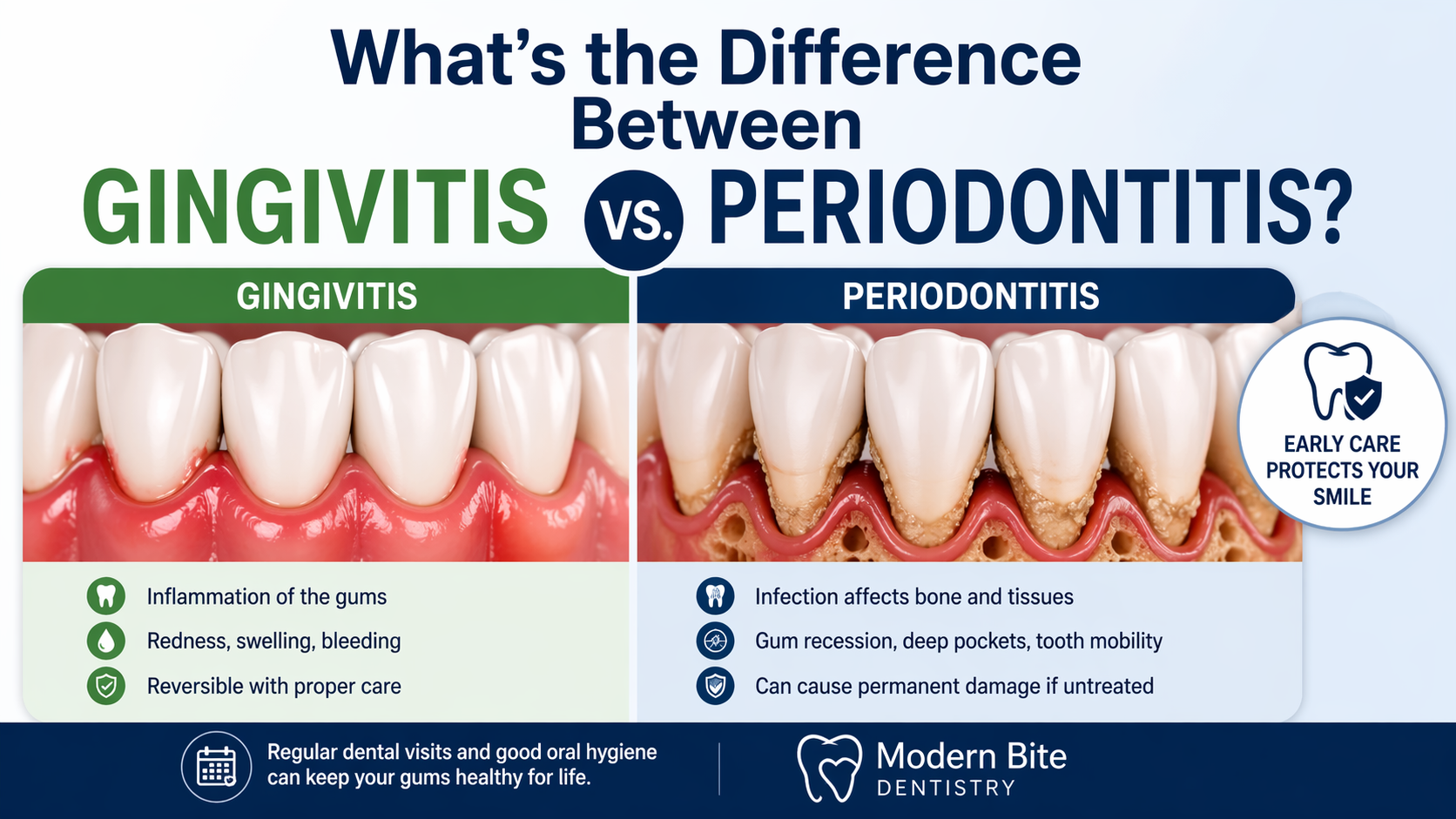
Gum disease is a common oral health condition that affects the tissues surrounding and supporting the teeth. It typically begins with mild inflammation of the gums and can progress into a more serious condition if not addressed. The two primary stages of gum disease are gingivitis and periodontitis, each with distinct characteristics, levels of severity, and long-term implications for oral health. Understanding how these conditions differ is important for recognizing early symptoms and preventing progression.
Gingivitis represents the initial stage of gum disease and is usually associated with plaque buildup along the gumline. At this stage, symptoms may include redness, swelling, and bleeding during brushing or flossing. If left untreated, gingivitis can develop into periodontitis, a more advanced condition that involves damage to the supporting bone and connective tissues. The progression from early inflammation to structural damage highlights the importance of timely intervention and consistent oral care.
Preventive care plays a key role in identifying and managing gum disease before it advances. Regular dental visits and professional cleanings help remove plaque and tartar that contribute to inflammation. Guidance on maintaining proper oral hygiene is often emphasized in resources such as how to treat prevent bleeding gums, which outlines strategies for reducing gum irritation and improving overall gum health.
As gum disease progresses, it can affect not only the gums but also the stability of the teeth and the underlying bone structure. Advanced cases may require more complex treatment to control infection and preserve oral function. Understanding the differences between gingivitis and periodontitis allows individuals to recognize when symptoms require professional evaluation and to take appropriate steps to protect long-term dental health.
Gingivitis and Periodontitis Explained
Gum disease develops as a result of bacterial accumulation along the gumline, but the severity and impact on oral structures vary significantly between its stages. Gingivitis and periodontitis represent two distinct phases of the same disease process, with differences in tissue involvement, reversibility, and long-term consequences. Identifying which stage is present allows for more accurate treatment planning and improved outcomes.
The transition from gingivitis to periodontitis is not always immediate, but it occurs when inflammation is left untreated over time. While gingivitis primarily affects the soft gum tissue, periodontitis extends deeper, impacting the bone and connective structures that support the teeth. Early diagnosis is critical because intervention at the gingivitis stage can often prevent permanent damage and reduce the need for more complex procedures.
What Is Gingivitis?
Gingivitis is the earliest stage of gum disease and is characterized by inflammation confined to the gum tissue. It develops when plaque accumulates along the gumline and triggers a localized inflammatory response. At this stage, the attachment between the gums and teeth remains intact, and there is no loss of supporting bone. This makes gingivitis a reversible condition when addressed with proper oral hygiene and professional care.
Common signs of gingivitis include redness, swelling, and bleeding during brushing or flossing. These symptoms may be mild and painless, which often leads to delayed treatment. However, the absence of pain does not indicate that the condition is harmless. Regular evaluation and preventive care services such as oral cancer screening often include assessment of gum health, allowing early-stage inflammation to be identified and managed before progression occurs.
What Is Periodontitis?
Periodontitis is a more advanced stage of gum disease that involves deeper infection and structural damage. As inflammation persists, the gums begin to separate from the teeth, forming pockets that trap bacteria and debris. These pockets create an environment where bacteria can thrive, leading to destruction of the connective tissue and bone that support the teeth.
Unlike gingivitis, periodontitis is not fully reversible because it involves permanent loss of supporting structures. Over time, this can result in gum recession, increased tooth mobility, and, in severe cases, tooth loss. Management of periodontitis focuses on controlling infection, slowing disease progression, and preserving as much of the remaining structure as possible.
How Gum Disease Progresses Over Time
The progression from gingivitis to periodontitis occurs gradually as plaque is not effectively removed. Bacteria within plaque produce toxins that irritate the gum tissue and trigger an inflammatory response. As this response continues, it begins to affect deeper tissues, breaking down the attachment between the gums and teeth.
Once periodontal pockets form, they become difficult to clean with routine brushing and flossing alone. This allows bacteria to multiply and accelerate tissue destruction. Without intervention, the cycle of inflammation and bacterial growth leads to progressive bone loss and weakening of tooth support. Understanding this progression highlights the importance of early detection and consistent preventive care.
Why Early Detection Matters
Early detection of gum disease significantly improves treatment outcomes. When gingivitis is identified in its initial stages, it can often be reversed through improved oral hygiene practices and professional cleaning. This prevents the need for more invasive procedures and helps maintain long-term oral health.
Routine dental visits play a key role in early diagnosis by allowing dentists to monitor changes in gum condition and detect subtle signs of disease progression. Preventive strategies, including regular examinations and patient education, are essential for reducing the risk of developing periodontitis. Early intervention not only preserves gum health but also helps protect the structural integrity of the teeth and supporting bone.
Key Differences Between Gingivitis and Periodontitis
Although gingivitis and periodontitis are part of the same disease process, they differ significantly in terms of severity, tissue involvement, and long-term impact on oral health. Gingivitis is limited to inflammation of the gum tissue, while periodontitis affects deeper structures, including connective tissue and bone. Understanding these differences is essential for determining appropriate treatment and preventing disease progression.
The distinction between these two stages also influences how they are managed clinically. Gingivitis can often be resolved with improved oral hygiene and professional cleaning, whereas periodontitis typically requires more advanced and ongoing treatment. Identifying the stage of gum disease early allows for more effective intervention and reduces the likelihood of permanent damage to the supporting structures of the teeth.
Symptoms and Clinical Signs
Gingivitis and periodontitis present with different clinical features, although some symptoms may overlap in the early stages. Gingivitis is commonly associated with red, swollen gums that bleed easily during brushing or flossing. These symptoms are usually localized to the gum tissue and do not involve deeper structures.
Periodontitis presents with more advanced signs, including gum recession, formation of periodontal pockets, and possible tooth mobility. Patients may also experience persistent bad breath or a bad taste in the mouth due to bacterial accumulation. In more severe cases, teeth may shift position as the supporting bone deteriorates. Recognizing these differences helps determine when professional intervention is required.
Reversibility and Long-Term Impact
One of the most important differences between gingivitis and periodontitis is reversibility. Gingivitis is generally reversible because it does not involve permanent damage to the bone or connective tissue. With proper oral hygiene and professional care, the inflammation can resolve and the gums can return to a healthy state.
Periodontitis, in contrast, involves irreversible damage. Once bone loss occurs, it cannot be fully restored through routine treatment. Management focuses on controlling infection, preventing further deterioration, and maintaining the remaining support structures. This distinction underscores the importance of early diagnosis and consistent preventive care to avoid progression beyond the reversible stage.
Tissue and Bone Involvement
Gingivitis affects only the superficial gum tissue, leaving the underlying bone and connective structures intact. The attachment between the gums and teeth remains stable, which is why the condition can be reversed with appropriate care.
Periodontitis involves deeper destruction, including breakdown of the periodontal ligament and loss of supporting bone. As the disease progresses, pockets form between the teeth and gums, creating spaces where bacteria accumulate. These changes weaken the structural support of the teeth and increase the risk of tooth loss over time. Comprehensive evaluation through services such as periodontal care is often necessary to assess the extent of damage and determine appropriate treatment.
Differences in Treatment Approach
Treatment strategies differ significantly between gingivitis and periodontitis due to the extent of tissue involvement. Gingivitis can typically be managed with professional cleaning and improved oral hygiene practices. Removing plaque and tartar allows the gum tissue to heal and reduces inflammation.
Periodontitis requires more intensive management to control infection and stabilize the condition. Treatment may include deep cleaning procedures, ongoing maintenance therapy, and monitoring of periodontal pockets. In some cases, additional interventions may be needed to preserve the remaining tooth structure. Regular preventive visits such as dental cleanings exams play an important role in both preventing progression and maintaining long-term gum health.
Causes and Risk Factors of Gum Disease
Gingivitis and periodontitis share the same primary cause, which is the accumulation of bacterial plaque along the gumline. Plaque is a sticky biofilm that forms continuously on tooth surfaces and contains bacteria capable of triggering inflammation in the surrounding gum tissue. When plaque is not effectively removed through daily oral hygiene, it can harden into tartar, which further promotes bacterial growth and makes cleaning more difficult.
While plaque is the initiating factor, several additional risk factors influence how quickly gum disease develops and how severe it becomes. Some individuals may experience mild inflammation that remains stable, while others progress more rapidly to advanced periodontal disease. Understanding these contributing factors helps guide both prevention and long-term management strategies.
Role of Plaque and Bacteria
Bacterial activity within plaque plays a central role in the development of gum disease. As plaque accumulates, bacteria release toxins that irritate the gum tissue and trigger an inflammatory response. In the early stages, this response leads to the redness and swelling associated with gingivitis.
If plaque is not removed, the bacterial load increases and begins to affect deeper tissues. The body’s immune response, combined with bacterial toxins, contributes to the breakdown of connective tissue and bone. This process marks the transition from gingivitis to periodontitis. Preventive measures, including professional cleanings and consistent oral hygiene, are essential for controlling bacterial buildup and reducing the risk of disease progression.
Lifestyle and Behavioral Factors
Certain lifestyle habits significantly increase the risk of developing gum disease or accelerating its progression. Smoking is one of the most important risk factors, as it reduces blood flow to the gums and impairs the body’s ability to respond to infection. Individuals who smoke may experience more severe periodontal damage with fewer noticeable early symptoms.
Diet and oral hygiene practices also play a role. Inconsistent brushing and flossing allow plaque to accumulate, while diets high in sugar can promote bacterial growth. Mechanical factors such as teeth grinding or clenching may place additional stress on the supporting structures of the teeth, contributing to tissue breakdown over time. Protective solutions such as night guards may be recommended in cases where grinding contributes to oral health complications.
Systemic and Medical Conditions
Systemic health conditions can influence the body’s response to bacterial infection and increase susceptibility to gum disease. Diabetes is a well-documented risk factor, as elevated blood sugar levels can impair immune function and delay healing. Individuals with uncontrolled diabetes are more likely to develop severe periodontal disease.
Hormonal changes, such as those occurring during pregnancy or menopause, can also affect gum sensitivity and increase inflammation. Additionally, certain medications may reduce saliva production, leading to dry mouth and increased bacterial accumulation. These factors highlight the importance of a comprehensive approach to oral health that considers both local and systemic influences.
Genetic and Environmental Influences
Genetic predisposition plays a role in how individuals respond to bacterial plaque and inflammation. Some people may be more susceptible to developing gum disease despite maintaining good oral hygiene. Environmental factors, including stress, can also influence immune response and contribute to disease progression.
Understanding the combination of genetic, environmental, and behavioral factors allows for more personalized prevention strategies. Regular dental evaluations help identify risk factors early and provide targeted recommendations to reduce the likelihood of progression from gingivitis to periodontitis.
Treatment Options for Gingivitis and Periodontitis
Treatment for gum disease depends on the stage and severity of the condition at the time of diagnosis. Gingivitis can typically be managed with non-invasive methods, while periodontitis often requires more advanced and ongoing care. The primary goal of treatment is to control bacterial infection, reduce inflammation, and prevent further damage to the supporting structures of the teeth.
Early intervention plays a significant role in treatment success. Addressing gingivitis promptly can prevent progression to periodontitis, reducing the need for complex procedures. As gum disease advances, treatment becomes more focused on long-term management rather than complete reversal, particularly when structural damage has already occurred.
Treating Gingivitis
Gingivitis treatment focuses on removing plaque and tartar buildup and improving daily oral hygiene habits. Professional dental cleaning is the primary approach used to eliminate accumulated deposits that cannot be removed through routine brushing and flossing. Once these irritants are removed, the gum tissue can begin to heal, and inflammation typically decreases.
In addition to professional cleaning, patients are advised to maintain consistent oral hygiene practices at home. This includes proper brushing technique, regular flossing, and the use of antimicrobial mouth rinses when recommended. Preventive measures and routine care, including services such as dental sealants, may also be discussed as part of a broader strategy to reduce bacterial accumulation and protect oral health.
Managing Periodontitis
Periodontitis requires a more comprehensive approach because it involves deeper infection and structural damage. Treatment often includes specialized cleaning procedures designed to remove plaque and tartar from below the gumline. These procedures help reduce bacterial presence within periodontal pockets and promote healing of the surrounding tissues.
Long-term management is an important aspect of periodontitis treatment. Patients may require regular maintenance visits to monitor gum health and prevent recurrence of infection. In some cases, additional therapies may be recommended to stabilize the condition and preserve remaining bone and connective tissue. Educational resources such as the importance of fluoride also highlight preventive strategies that support overall oral health and reduce the risk of further complications.
Professional Maintenance and Monitoring
Ongoing monitoring is essential for both gingivitis and periodontitis, especially for individuals with a history of gum disease. Regular dental visits allow for early detection of changes in gum condition and help ensure that treatment remains effective over time. Maintenance care focuses on controlling plaque levels and preventing the reestablishment of harmful bacteria.
Patients with periodontitis may require more frequent visits compared to those with healthy gums. These visits typically involve professional cleaning, evaluation of periodontal pockets, and assessment of overall oral health. Consistent follow-up care helps reduce the risk of disease progression and supports long-term stability.
Preventive Strategies for Long-Term Gum Health
Preventing gum disease involves a combination of professional care and daily oral hygiene practices. Brushing twice daily, flossing regularly, and maintaining a balanced diet all contribute to reducing plaque accumulation. Avoiding risk factors such as smoking further supports gum health and improves the body’s ability to respond to bacterial challenges.
Preventive dental services play a central role in maintaining healthy gums and teeth. Regular checkups provide an opportunity to identify early signs of inflammation and implement corrective measures before the condition progresses. By combining preventive care with appropriate treatment, individuals can significantly reduce the risk of developing advanced periodontal disease.
When to See a Dentist for Gum Disease
Recognizing when to seek professional dental care is essential for preventing gum disease from progressing. Early symptoms such as bleeding during brushing, mild gum swelling, or persistent bad breath may indicate the presence of gingivitis. These signs are often overlooked because they may not cause significant discomfort, but they reflect underlying inflammation that requires attention.
As gum disease advances, symptoms may become more noticeable and indicate deeper tissue involvement. Gum recession, increased tooth sensitivity, or a feeling that teeth are becoming loose may suggest progression to periodontitis. At this stage, professional evaluation is necessary to assess the extent of damage and determine an appropriate treatment plan. Early intervention reduces the likelihood of long-term complications and helps preserve the supporting structures of the teeth.
Signs You Should Not Ignore
Certain symptoms require prompt dental evaluation because they may indicate active infection or structural damage. Persistent bleeding, swollen or tender gums, and discomfort while chewing are common warning signs. In more advanced cases, visible gum recession or changes in tooth alignment may occur as the supporting tissues weaken.
Ignoring these symptoms allows the condition to progress and increases the risk of irreversible damage. Timely diagnosis enables targeted treatment that can control infection and stabilize gum health before more invasive procedures become necessary.
Importance of Early Diagnosis
Early diagnosis plays a critical role in managing both gingivitis and periodontitis. When gum disease is identified at an early stage, treatment is typically less complex and more effective. Addressing gingivitis promptly can prevent progression to periodontitis, reducing the need for long-term management and preserving natural tooth support.
Regular dental visits provide an opportunity to detect subtle changes in gum condition that may not be noticeable at home. Professional evaluation includes assessment of gum health, measurement of periodontal pockets, and identification of risk factors that may contribute to disease progression.
Long-Term Benefits of Preventive Care
Consistent preventive care supports long-term gum health and reduces the likelihood of developing advanced periodontal disease. Routine examinations and professional cleanings help control plaque levels and maintain healthy gum tissue. Preventive strategies also include patient education on proper oral hygiene techniques and lifestyle modifications.
Maintaining healthy gums contributes to overall oral stability and reduces the risk of tooth loss. Long-term monitoring ensures that any changes in gum condition are addressed promptly, supporting sustained oral health and function.
If you are experiencing symptoms such as bleeding gums, persistent bad breath, or gum sensitivity, scheduling a professional evaluation can help identify the underlying cause. Early assessment allows for accurate diagnosis and timely treatment, which can prevent the progression from gingivitis to periodontitis.
Modern Bite Dentistry provides comprehensive care for all stages of gum disease, from early prevention to advanced periodontal management. Patients seeking evaluation or treatment can schedule an appointment through the clinic’s contact page to receive personalized care and guidance tailored to their oral health needs.

